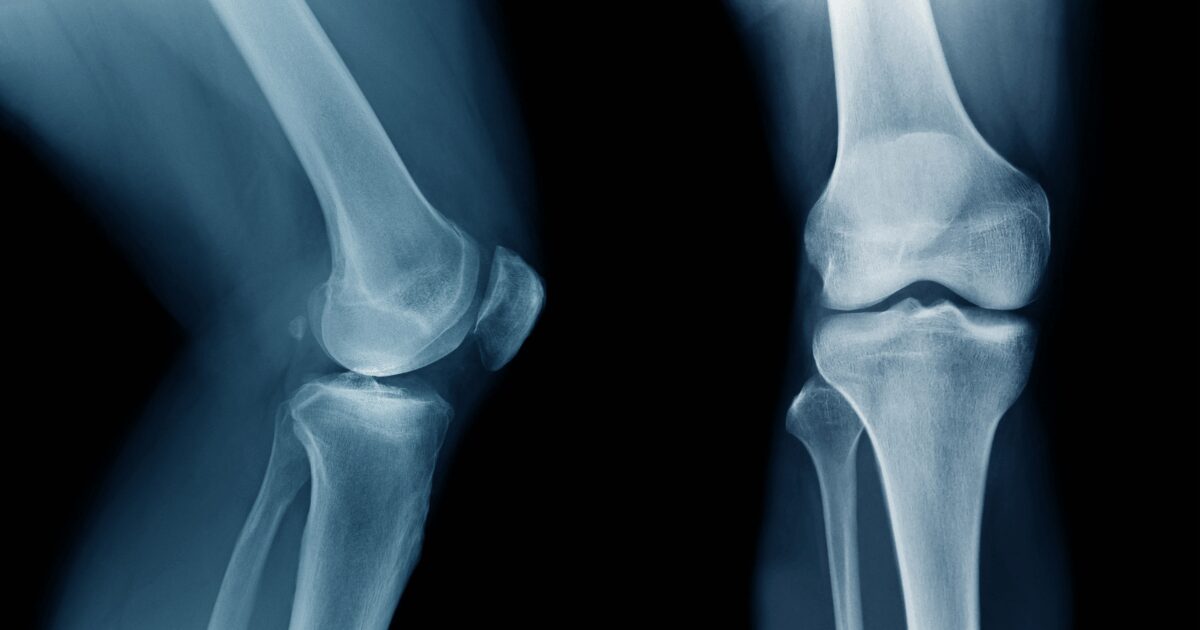
Does Menopause Cause Osteoporosis?
Learn how to protect your bone health today.
Does Menopause Cause Osteoporosis?
Learn how to protect your bone health today.
Osteoporosis isn’t just about bones, it’s about your whole health. That’s why Dr. Polly Watson says,
“Osteoporosis is a disease that weakens bones, increasing the risk of sudden and unexpected fractures.”
And for menopausal women, the risk becomes even more real.
In fact, 40% of women over 50 will break a bone due to osteoporosis, and many won’t even know they’re at risk until it happens.
In this episode of Menopause Rescue, Dr. Polly Watson explores osteoporosis in women over 50, shedding light on why it’s a critical yet often overlooked aspect of women’s health during and after menopause. Dr. Watson shares personal experiences and expert insights on the complex factors that affect bone health, including hormonal changes, medications, lifestyle habits, and nutrition.
Watch The Conversation!
Key Takeaways:
- Bone thinning (osteoporosis) is common and serious for women over 50. It has many causes, not just a lack of calcium, and breaking a hip can be very dangerous.
- Bone density scans (DEXAs) alone don’t always show who will break a bone. Doctors also need to look at your family’s health history, the medicines you take, and your chances of falling.
- Some common medicines can make bones weaker. These include certain antidepressants (SSRIs), pills for stomach acid (PPIs), and steroids, making breaks more likely.
- You can help your bones by living healthy. Eat enough protein, have a good diet, do exercises that build strength and balance, get at least 7 hours of sleep, manage stress, and avoid alcohol and smoking.
- Hormone Replacement Therapy (HRT) can lower your risk of breaking bones after menopause. Talk to your doctor to see if this is a good option for keeping your bones strong.
Osteoporosis isn’t just about bones, it’s about your whole health. That’s why Dr. Polly Watson says,
“Osteoporosis is a disease that weakens bones, increasing the risk of sudden and unexpected fractures.”
And for menopausal women, the risk becomes even more real.
In fact, 40% of women over 50 will break a bone due to osteoporosis, and many won’t even know they’re at risk until it happens.
Quotes:
- “Osteoporosis affects nearly half of women over 50. And it’s not just a bone issue—it’s a whole person issue.” Dr. Polly Watson
- “Calcium alone has not been shown to improve bone mineral density.” Dr. Polly Watson
- “This is a time to not just focus on preventing fractures, but to move through your life with energy, strength, and confidence.” Dr. Polly Watson
Resources:
Resources: https://hormonewellnessmd.com/podcast-resources
Disclaimer: https://hormonewellnessmd.com/podcast#Disclaimer
How Menopause Increases the Risk of Osteoporosis
“Estrogen protects your bones. Menopause triggers bone loss,” Dr. Watson explains. As estrogen levels decline, the balance between bone formation and bone resorption shifts, and not in your favor. This leads to a drop in bone mineral density (BMD), particularly in the first five years after menopause.
According to Dr. Watson, “Women lose about 50% of their trabecular bone and 30% of their cortical bone during the course of their lifetime.” That’s why postmenopausal osteoporosis is so common and why early action matters.
She warns that menopause-related bone loss is often missed because “osteoporosis is often called a ‘silent disease’, initially bone loss occurs without symptoms.”
Can You Prevent Bone Loss During Menopause?
While hormonal changes put you at a disadvantage, your daily choices can tip the scale. Dr. Watson emphasizes that bone health is a “complex symphony” involving sex hormones, stress hormones (like cortisol), thyroid function, sleep, exercise, nutrition, and medications.
And it starts earlier than you might think.
“You do not have to wait until you’re postmenopausal to start hormone replacement therapy,” she says. “If you’re symptomatic – hot flashes, night sweats – your estrogen levels are fluctuating enough that you’re probably also losing some bone mass.”
That means even perimenopausal women should be thinking about osteoporosis prevention.
Why Ignoring Bone Health Can Be Dangerous
The consequences of ignoring bone health can be life-changing or even life-threatening.
“Once a person breaks their hip, particularly if they’re over 65, that often translates into months of rehab, loss of independence, and… a 20% chance of death within the first year,” says Dr. Watson. “You’re more likely to die after a hip fracture than you are from breast cancer.”
And if you survive? “Thirty percent never recover their pre-fracture level of ability.”
This is why fracture risk assessment and prevention are so crucial for postmenopausal women.
How Reliable Are DEXA Scans for Fracture Risk?
The most common screening tool for osteoporosis is a DEXA scan, but Dr. Watson wants women to know its limitations: “Half of women who fracture have a normal DEXA scan.”
In other words, even with a normal result, you may still be at risk. That’s why she looks beyond just bone density numbers. She urges women to also consider:
- Family history of fractures
- Personal fracture history
- Fall risk and balance
Medication use (especially SSRIs, steroids, and PPIs) - Lifestyle factors like smoking, alcohol consumption, and inactivity
How Hormone Therapy Protects Bone Density
“Hormone therapy is believed to be useful in preventing bone loss that leads to osteoporosis,” says Dr. Watson. Research backs this up. “Menopause hormone therapy (MHT) has been shown to significantly increase bone mineral density.”
Fracture risk reductions with MHT:
- 27% fewer total fractures
- 33% fewer hip fractures
- 37% fewer spine fractures
However, she cautions that stopping hormone therapy can quickly reverse those gains: “Most increased BMD disappears within a few years.”
This is why Dr. Watson emphasizes shared decision-making with your provider, especially for recently postmenopausal women, about how long to continue hormone replacement therapy.
How to Build and Maintain Healthy Bones Naturally
Dr. Watson is clear: hormone therapy isn’t the only answer. There’s a lot you can do without medication to prevent bone loss and even rebuild bone:
Eat for your bones
“Adequate amounts of calcium should be included in the diet,” she advises, ideally from whole foods. Caution with calcium supplementation. You can only absorb about 400 – 600 mg of calcium at a time. If you supplement and eat dairy, you may be taking in more than you can actually absorb. Think dark green leafy vegetables, salmon, tofu, and fortified plant milks. She adds that vitamin D and K2 are also essential “to use calcium properly” and keep it going into bones, not arteries.
Get enough protein
“Nutrition, especially adequate protein intake, plays a vital role in the accumulation of peak bone mass,” says Dr. Watson. She recommends aiming for “a gram per pound of ideal body weight,” especially if you’re lifting weights or trying to build muscle.
Move with purpose
“Regular weight-bearing exercise helps build strong bones and may prevent osteoporosis.” Dr. Watson encourages women to do the following exercises to strengthen bone tissue and reduce fall risk:
- Strength training and resistance work
- Single-leg and balance exercises (e.g., tree pose, curtsy squats)
- Agility and functional movement to prevent falls
Sleep and stress matter
“Women who slept less than seven hours a night had greater poor bone mineral density,” she says. “Stress hormone degrades bone.” So managing cortisol levels through yoga, mindfulness, and rest isn’t just good for your mood, it’s crucial for your skeleton. Chronic stress can also sometimes lead to adrenal dysfunction.
Avoid bone-harming habits
Dr. Watson doesn’t mince words: “Smoking can increase the risk of osteoporosis by decreasing the body’s estrogen levels.” And even just “two servings of alcohol a day increases your fracture risk.”
Common medications that contribute to bone loss include:
- SSRIs and anti-anxiety medications
- Sleep aids (e.g., Ambien)
- Steroids for autoimmune disease
- Acid blockers like PPIs
She also urges caution with medications that may quietly undermine your bone strength. Talk with your doctor about alternatives if you’re on long-term medications.
You’re Not Fragile, You’re in Control
“Osteoporosis is the most common kind of bone disease and may progress without symptoms,” says Dr. Polly Watson. But menopause doesn’t have to mean weaker bones.
“This is a time to not just focus on preventing fractures, but to move through your life with energy, strength, and confidence.”
By eating well, staying active, supporting your hormones, and understanding your risk factors, you can protect your bone density and prevent fractures. The earlier you start, the stronger your future.
Want expert guidance on protecting your bones through menopause? Visit Hormone Wellness MD to explore personalized care that supports your strength, balance, and long-term health.
FAQ
Does menopause cause osteoporosis or increase the risk of bone loss?
Menopause can lead to faster bone loss because estrogen levels drop. Estrogen helps keep bones strong. Without it, bones can weaken, making fractures more likely.
Why is osteoporosis often referred to as a “silent disease”?
Osteoporosis often goes unnoticed until a bone breaks. Bones slowly lose density, but symptoms are rare. This is why checking for bone health is so important.
How do hormonal changes affect bone health during and after menopause?
Without enough estrogen, bones break down faster than they’re made. This is common in menopause. Eating right, exercising, and talking to a doctor can help keep bones strong.
Which risk factors make someone more likely to develop osteoporosis?
Age, low weight, family history, smoking, and alcohol use are big risks. Early menopause and certain health issues also increase risk. These factors can weaken bones and raise fracture risk.
How can I slow bone loss and maintain healthy bones during menopause?
Healthy habits are key. Exercise, eat enough calcium and vitamin D3 and K2, and limit alcohol. A balanced diet and, if needed, medication can also help.
What role does hormone replacement therapy play in managing menopausal bone loss?
Hormone therapy can help by replacing lost estrogen. This can slow bone loss and reduce fracture risk. But, it’s not right for everyone due to possible side effects. Always talk to a doctor first.
When should a fracture risk assessment be done?
A risk assessment is recommended at menopause or if there are other risk factors. Tests like a DEXA scan can detect bone issues early. This allows for early treatment to prevent fractures.
Which nutrients support osteoporosis prevention in postmenopausal women?
Calcium and vitamin D are essential for bone health. They help absorb calcium and keep bones strong. A diet rich in dark greens and protein, along with exercise and less alcohol, supports bone health. To make the biggest impact, I’d recommend a whole foods diet plus exercise, stress management, community, and quality sleep rather than taking lots of supplements.
Meet the host!
Dr. Polly Watson is a board certified OBGYN who has additional training in menopausal medicine, sexual medicine and functional medicine.
She looks forward to sharing her knowledge with you to help find a solution to address the imbalance in your system and restore your health.
In 2019 I left my job as an employed physician with a large organization and started Hormone Wellness MD. I started with no staff working out of a single room. Since then, my staff has grown to a team of 5 and we’ve helped over 1,100 people on their health journey.

Meet the host!

Dr. Polly Watson is a board certified OBGYN who has additional training in menopausal medicine, sexual medicine and functional medicine.
She looks forward to sharing her knowledge with you to help find a solution to address the imbalance in your system and restore your health.
In 2019 I left my job as an employed physician with a large organization and started Hormone Wellness MD. I started with no staff working out of a single room. Since then, my staff has grown to a team of 5 and we’ve helped over 1,100 people on their health journey.